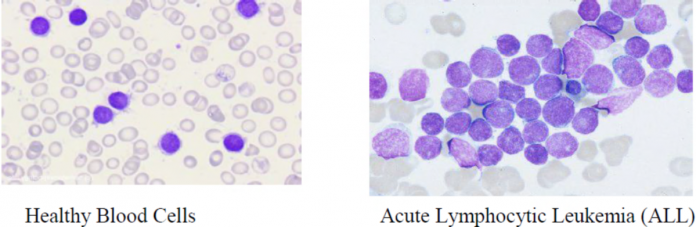
Acute Lymphocytic Leukemia (ALL) is a kind of blood most cancers that begins within the bone marrow and grows rapidly if left untreated. It primarily impacts kids however can even happen in adults, the place outcomes are sometimes much less favorable. In ALL, the physique makes too many immature white blood cells referred to as lymphoblasts, which crowd out wholesome cells and disrupt regular blood perform. Over time, it will probably unfold to organs just like the mind, liver, and spleen. Due to advances in analysis, therapies have improved—however challenges like relapse and therapy unintended effects stay. On this put up, we’ll discover what makes ALL so advanced.
Introduction
Acute lymphocytic leukemia (ALL) is an aggressive hematologic malignancy characterised by the clonal proliferation of immature lymphoid precursors, or lymphoblasts, within the bone marrow, blood, and different organs. Whereas predominantly a pediatric most cancers, with a peak incidence between ages 2 and 5, ALL additionally impacts adults and presents distinctive challenges throughout age teams.
For researchers and trainees within the biomedical sciences, understanding the molecular and mobile mechanisms of ALL is foundational for contributing to ongoing developments in analysis, danger stratification, and therapy. This text provides a research-centered overview of ALL, specializing in pathogenesis, classification, and evolving therapeutic methods.
Pathogenesis and Mobile Origin
ALL originates from lymphoid progenitor cells within the bone marrow that purchase genetic and epigenetic alterations, disrupting regular differentiation and selling uncontrolled proliferation. These cells might decide to both the B-cell or T-cell lineage, with B-ALL being the predominant subtype in kids and T-ALL extra frequent in adolescents and younger adults.
Molecular alterations sometimes contain:
-
Transcription issue dysregulation (e.g., PAX5, IKZF1, ETV6)
-
Aberrant kinase signaling (e.g., ABL1, JAK2, FLT3)
-
Chromosomal translocations (e.g., t(12;21)[ETV6-RUNX1], t(9;22)[BCR-ABL1])
-
Copy quantity abnormalities (e.g., deletions in CDKN2A, IKZF1)
These mutations drive leukemogenesis by enhancing self-renewal, impairing apoptosis, and blocking differentiation. In T-ALL, activation of the NOTCH1 pathway is a central oncogenic occasion, noticed in over 50% of circumstances.
Epidemiology and Danger Elements
-
Incidence: ~4,000 new circumstances yearly within the U.S.
-
Age Distribution: Bimodal peak—kids (2–5 years) and older adults (>50 years)
-
Intercourse: Slight male predominance
-
Ethnicity: Larger incidence in White populations
Recognized Danger Elements
-
Genetic syndromes: Trisomy 21 (Down syndrome), Bloom syndrome, Ataxia telangiectasia, Fanconi anemia, Li-Fraumeni syndrome
-
Excessive-dose radiation publicity
-
Earlier chemotherapy (alkylating brokers, topoisomerase inhibitors)
-
Inherited mutations in DNA restore or cell cycle genes
Classification and Molecular Subtypes
WHO 2022 Classification of ALL:
B-lymphoblastic leukemia/lymphoma (B-ALL):
T-lymphoblastic leukemia/lymphoma (T-ALL):
Molecular profiling is now important not just for analysis however for figuring out actionable targets (e.g., ABL-class fusions, JAK-STAT activation, CRLF2 rearrangements).
Scientific Presentation
Signs come up from marrow failure, leukemic infiltration, and metabolic dysregulation:
-
Marrow failure: Anemia, thrombocytopenia, neutropenia → fatigue, bleeding, an infection
-
Organ infiltration: Hepatosplenomegaly, lymphadenopathy, bone ache
-
CNS involvement: Headache, vomiting, cranial nerve palsies
-
Metabolic: Hyperuricemia, hyperkalemia, tumor lysis syndrome
These non-specific signs typically mimic viral infections or autoimmune situations, necessitating immediate hematologic analysis.
Analysis and Work-Up
Preliminary Analysis:
-
CBC and peripheral smear: Elevated WBCs with lymphoblasts, anemia, thrombocytopenia
-
Bone marrow aspiration/biopsy: ≥20% lymphoblasts defines ALL (per WHO)
-
Movement cytometry: Immunophenotyping to categorise B- vs. T-lineage and maturation stage
-
Cytogenetics/FISH: Detection of translocations (e.g., t(9;22), t(4;11))
-
Molecular assays: RT-PCR or NGS to detect fusion transcripts or mutations
-
Lumbar puncture: To evaluate CNS involvement
-
MRD evaluation: Measured by movement cytometry or qPCR post-induction
Minimal residual illness (MRD) is now a cornerstone biomarker for therapy response and danger stratification.

Remedy Overview
1. Induction Section (~4 weeks)
Purpose: Obtain full remission (CR) by eliminating >99% of leukemic cells
Medication: Vincristine, corticosteroids, L-asparaginase, ± anthracyclines
CNS prophylaxis is initiated by way of intrathecal methotrexate/cytarabine
2. Consolidation/Intensification Section
Purpose: Eradicate residual illness and stop systemic/CNS relapse
Contains high-dose methotrexate, cytarabine, and additional intrathecal chemo
3. Upkeep Section (2–3 years)
Purpose: Suppress late-emerging clones
Day by day 6-mercaptopurine, weekly methotrexate, periodic vincristine/steroids
4. CNS Prophylaxis
Common, given excessive danger of CNS relapse. Might contain intrathecal chemo ± cranial irradiation (in choose high-risk circumstances)
Focused and Immunotherapies
Tyrosine Kinase Inhibitors (TKIs)
-
For Ph+ ALL: Imatinib or dasatinib with chemo considerably improves outcomes
-
Newer TKIs (e.g., ponatinib) utilized in T315I mutant circumstances
CAR-T Cell Remedy
-
CD19-directed CAR-T (e.g., tisagenlecleucel) achieves MRD-negative remissions in relapsed/refractory B-ALL
-
Main hostile results: cytokine launch syndrome (CRS), immune effector cell–related neurotoxicity syndrome (ICANS)
Bispecific T-cell Engagers (BiTEs)
Antibody-Drug Conjugates
-
Inotuzumab ozogamicin: Anti-CD22 ADC utilized in relapsed/refractory B-ALL
-
Related to veno-occlusive illness, particularly post-transplant
JAK-STAT Pathway Inhibition
Prognostic Elements
Favorable:
-
Age 1–10 years
-
WBC
-
Hyperdiploidy
-
ETV6-RUNX1 fusion
-
Speedy MRD clearance
Unfavorable:
MRD negativity (
Challenges and Rising Instructions in Analysis
-
Relapsed/refractory ALL stays a serious impediment; molecular profiling guides salvage methods.
-
Lineage plasticity and antigen escape (e.g., CD19 loss post-CAR-T) pose therapeutic challenges.
-
Clonal evolution underneath selective strain from remedy highlights the necessity for longitudinal genomic monitoring.
-
Bettering outcomes in adults and high-risk subgroups (e.g., T-ALL, hypodiploid B-ALL) requires additional translational analysis.
-
Epigenetic dysregulation (e.g., CREBBP, NSD2) and metabolic vulnerabilities supply potential new targets.
-
Subsequent-gen immunotherapies (e.g., trispecific antibodies, dual-target CARs) are in early scientific improvement.
Conclusion
Acute lymphocytic leukemia serves as a mannequin illness for understanding clonal evolution, focused remedy, and immune-oncology. Regardless of vital enhancements in pediatric survival charges, unmet wants stay in grownup populations and relapsed illness. As analysis continues to dissect the genetic, epigenetic, and microenvironmental drivers of ALL, future therapies will probably grow to be more and more customized.
For medical analysis trainees, ALL provides a wealthy platform for research—spanning stem cell biology, immunotherapy, programs genomics, and drug resistance. Continued collaboration between clinicians and scientists shall be vital to advancing outcomes for all sufferers affected by this aggressive leukemia.