Most cancers is without doubt one of the most complicated and instructive human ailments, representing a dramatic disruption of regular mobile processes that enables cells to develop uncontrollably, resist dying, invade surrounding tissues, and metastasize. With the incidence of most cancers rising worldwide, understanding its underlying mechanisms is essential for college students, researchers, and clinicians. Many years of analysis have revealed that most cancers might be understood via distinct however interconnected conceptual dimensions, together with:
-
Acquired useful capabilities (hallmarks of most cancers)
-
Enabling phenotypic traits
-
Hallmark-conveying cells within the tumor microenvironment (TME)
-
Systemic interactions throughout the host
Collectively, these dimensions present a framework to review most cancers as a dynamic, adaptive “outlaw organ”, guiding the event of therapeutic methods.
Introduction: The Hallmarks Idea
The idea of “hallmarks of most cancers” was launched by Douglas Hanahan and Bob Weinberg to arrange the huge variety of genetic and phenotypic adjustments noticed in tumors. The purpose was to know how cancers come up via multistep tumorigenesis, evolve via selective pressures, and purchase traits similar to metastasis, remedy resistance, and immune evasion.
Timeline of hallmark evolution:
-
2000: Six hallmarks: sustaining proliferative signaling, evading development suppressors, resisting cell dying, replicative immortality, angiogenesis, invasion/metastasis.
-
2011: Added deregulated metabolism and immune evasion.
-
2022: Phenotypic plasticity added, emphasizing dynamic adaptation to remedy and atmosphere.
A central realization was that mutant most cancers cells alone don’t outline tumor biology. As a substitute, most cancers development is determined by recruitment and reprogramming of surrounding regular cells, making a supportive tumor microenvironment (TME).
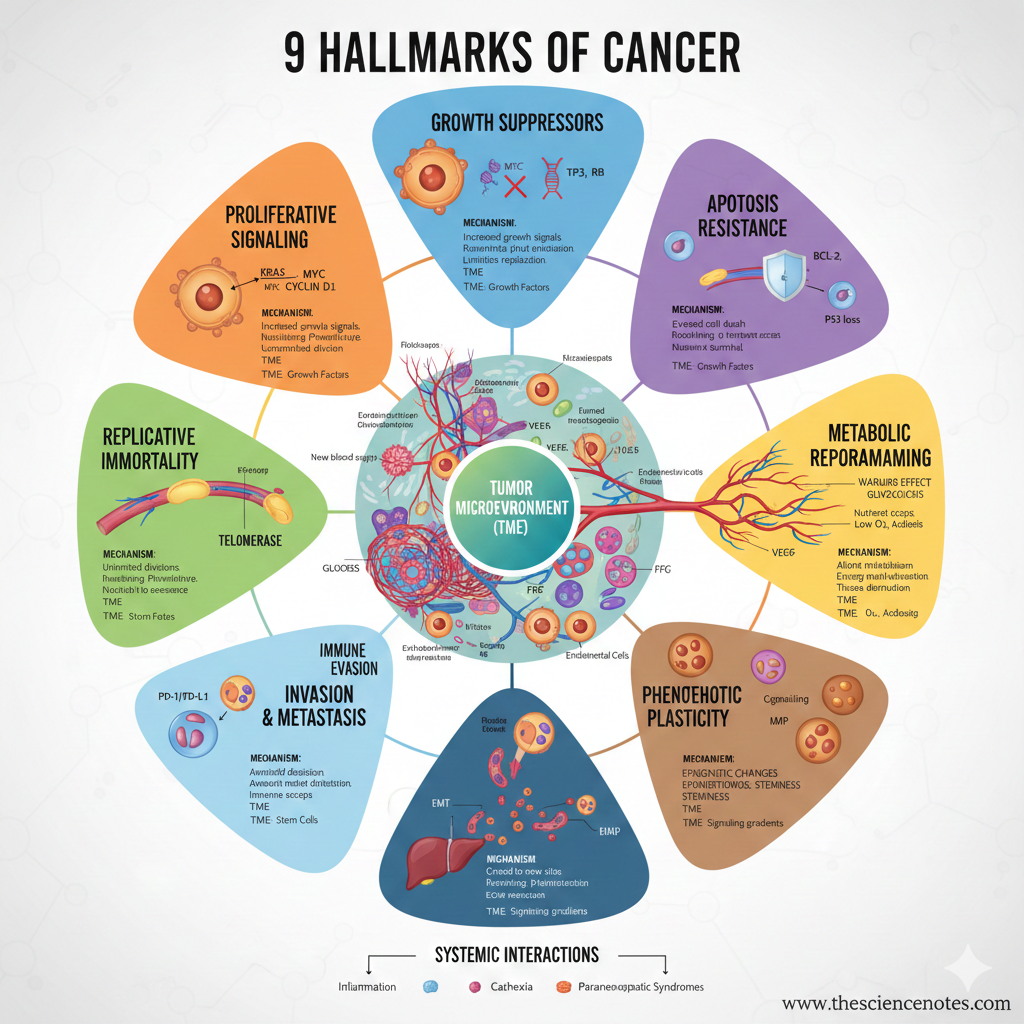
The 9 Hallmarks of Most cancers
1. Sustaining Proliferative Signaling
Most cancers cells obtain uncontrolled proliferation by activating oncogenes, which drive continual cell cycle development.
Key oncogenes:
-
KRAS, NRAS, HRAS: Mutations in KRAS are seen in ~30% of tumors, together with pancreatic (~90%), colorectal (~50%), and lung (~35%) cancers.
-
BRAF, PIK3CA, BCR-ABL: Drive aberrant development indicators.
-
MYC: Transcription issue regulating hundreds of genes; amplified in ~40% of tumors.
Mechanisms:
-
Gene amplification or rearrangement
-
Round extrachromosomal DNA (ecDNA) enhancing oncogene expression
-
Epigenetic reprogramming, together with autocrine/paracrine development issue loops
Medical relevance: Focused therapies embody BRAF inhibitors (vemurafenib) and HER2 inhibitors (trastuzumab).
Extra perception: RAS and MYC can stimulate a number of different hallmark capabilities, together with metabolic reprogramming and angiogenesis, highlighting their centrality in tumor evolution.
2. Evading Progress Suppressors
Regular cells regulate proliferation by way of tumor suppressor genes (TSGs), which act as gatekeepers for cell cycle checkpoints.
Key TSGs:
-
TP53: Activated in response to DNA harm, oncogenic stress, or hypoxia; regulates apoptosis, senescence, and cell-cycle arrest. Mutated in ~40% of cancers.
-
RB, CDKN1A/B (p21/p27), CDKN2A (p16INK4a/p14ARF): Block development via G1/S and G2/M transitions.
-
APC: Degrades β-catenin to forestall uncontrolled proliferation.
Mechanisms of evasion:
Medical relevance: Medication like CDK inhibitors (palbociclib, ribociclib) can restore development suppression in tumors with TSG inactivation.
3. Resisting Programmed Cell Demise (Apoptosis)
Most cancers cells evade mobile suicide mechanisms, enabling survival regardless of DNA harm or irregular signaling.
Mechanisms:
-
Overexpression of anti-apoptotic proteins: BCL-2, BCL-XL, MCL-1
-
TP53 inactivation, stopping induction of pro-apoptotic genes like PUMA and NOXA
-
Dysregulation of different cell dying pathways: necroptosis, ferroptosis, pyroptosis, autophagy
Therapeutics: BH3 mimetics (Venetoclax) restore apoptosis in CLL and AML, with ongoing trials in different cancers.
Paradoxical perception: Apoptotic cells can stimulate tumor-promoting indicators in neighboring cells or escape dying with partially broken genomes, contributing to genomic instability and tumor development.
4. Establishing Replicative Immortality
Regular cells are restricted by a mitotic clock dictated by telomere size. Most cancers cells bypass this to divide indefinitely.
Mechanisms:
-
Telomerase activation (TERT): Provides telomere repeats, widespread in glioblastoma (~80%), melanoma (~60%), bladder most cancers (~80%).
-
Different Lengthening of Telomeres (ALT): Recombination-based telomere extension, widespread in mesenchymal and neuroepithelial tumors.
Penalties:
5. Inducing or Accessing Vasculature (Angiogenesis)
Tumors require oxygen and vitamins to develop past 1–2 mm.
Mechanisms:
-
Hypoxia triggers VEGFA, ANGPT2, and FGF secretion
-
Endothelial cell activation, sprouting, and capillary formation
-
Recruitment of pericytes for vessel stabilization
Tumor vasculature:
-
Leaky, chaotic, and poorly perfused
-
Impedes immune cell infiltration, contributing to immune evasion
Different mechanism: Vascular co-option, the place tumors hijack pre-existing vessels, significantly after anti-angiogenic remedy.
Medical relevance: Anti-angiogenic remedy (e.g., bevacizumab) targets VEGF pathways.
6. Deregulating Mobile Metabolism
Most cancers cells reprogram metabolism to meet vitality and biosynthetic calls for.
Metabolic methods:
-
Cardio glycolysis (Warburg impact) alongside oxidative phosphorylation
-
Utilization of different fuels: lactate, glutamine
-
Metabolic crosstalk with tumor microenvironment cells (fibroblasts, macrophages, T cells)
TME components:
-
Hypoxia, acidosis, nutrient gradients
-
Paracrine secretion of metabolites
-
Dynamic diversifications throughout tumor development and metastasis
Therapeutic implications: Concentrating on glycolysis or glutamine metabolism can disrupt tumor development.
7. Activating Invasion and Metastasis
Most cancers cells purchase the flexibility to unfold past their origin.
Mechanisms:
-
Epithelial-to-mesenchymal transition (EMT) → motility
-
Extracellular matrix transforming by way of MMPs
-
Entry into blood or lymphatic circulation
-
Colonization of distant organs
TME contribution: Stromal cells and immune cells secrete components facilitating invasion.
Medical significance: Metastasis causes ~90% of cancer-related deaths.
8. Evading Immune Destruction
Tumors escape immune surveillance by way of:
-
Immune checkpoints (PD-L1, CTLA-4)
-
Immunosuppressive cytokines
-
Transforming of tumor vasculature to forestall T-cell infiltration
Therapeutics: Checkpoint inhibitors (nivolumab, pembrolizumab) restore T-cell exercise.
9. Unlocking Phenotypic Plasticity
Most cancers cells dynamically change between proliferative, invasive, and drug-resistant states.
Significance:
-
Drives remedy resistance, relapse, and metastasis
-
Permits adaptation to fluctuating TME and systemic pressures
Enabling Phenotypic Traits
These assist the acquisition of hallmarks:
-
Genomic instability: accelerates mutations and tumor evolution
-
Tumor-promoting irritation: sure immune cells facilitate development
-
Epigenetic transforming and oxidative stress adaptation improve survival underneath antagonistic circumstances
Tumor Microenvironment (TME)
Tumors are heterogeneous “organs” with a number of interacting cell varieties:
-
Most cancers cells: proliferate and adapt
-
Fibroblasts: transform ECM and secrete development components
-
Immune cells: suppress or promote tumor development
-
Blood vessels: ship vitamins and take away waste
Position: The TME contributes to development, invasion, angiogenesis, immune evasion, metabolic adaptation, and remedy resistance.
Systemic Interactions
Tumors work together with the physique systemically, altering:
-
Hormone ranges
-
Metabolic stability
-
Immune surveillance
Impression: Systemic results affect tumor development and remedy response.
Therapeutic Implications
Efficient most cancers remedy typically requires multi-hallmark concentrating on:
-
Oncogene inhibitors: KRAS, BRAF, HER2
-
Tumor suppressor modulators: CDK inhibitors
-
Apoptosis activators: BH3 mimetics
-
Anti-angiogenic medicine: VEGF inhibitors
-
Immunotherapy: checkpoint inhibitors
-
Metabolic inhibitors: glycolysis/glutamine concentrating on
Mixture remedy is essential to beat plasticity, adaptation, and resistance.
-
Hanahan, D., & Weinberg, R. A. (2011). Hallmarks of most cancers: The subsequent era. Cell, 144(5), 646–674. https://doi.org/10.1016/j.cell.2011.02.013
-
Hanahan, D. (2022). Hallmarks of most cancers: New dimensions. Most cancers Discovery, 12(1), 31–46. https://doi.org/10.1158/2159-8290.CD-21-1059
-
Hanahan, D. (2026). Hallmarks of most cancers—Then and now, and past. Cell. https://doi.org/10.1016/j.cell.2025.12.049

